Meningitis vaccines could help improve protection against gonorrhea amid rising cases globally and increasing bacterial resistance to drugs used to treat the infection, according to findings from three linked papers published in The Lancet Infectious Diseases journal.
Gonorrhea is a sexually transmitted infection (STI) which, if untreated, can lead to serious health conditions, including infertility in women, transmission to newborn babies, and increased risk of HIV. More than 80 million new cases of gonorrhea were recorded worldwide in 2020.
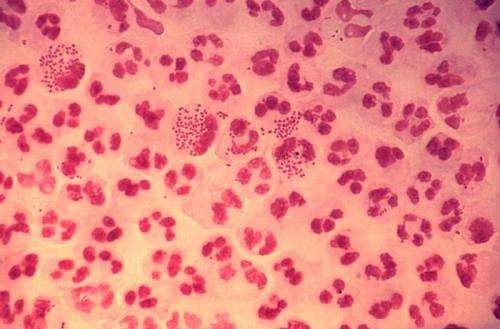
Declining effectiveness of drug treatments for the bacteria responsible—Neisseria gonorrhoeae—and the lack of a licensed vaccine to prevent the infection have raised concerns about the possibility that gonorrhea may become more resistant to treatment, or even untreatable, in future.
Meningitis vaccines have been recommended by the WHO as part of its roadmap to reduce the global burden of meningitis. This includes offering meningitis vaccines as part of routine childhood immunization strategies. Since meningitis vaccines have become more widely available, studies have shown they also offer some protection against gonorrhea, and that even partial protection could reduce cases of the infection considerably. However, questions have remained about the impacts and effectiveness of using meningitis vaccines against gonorrhea.
In 2016, the WHO set a target to reduce gonorrhea incidences by 90% by 2030, however an effective vaccine has yet to be developed. The three studies suggest that the 4CMenB vaccine may offer significant protection to young adults, and to men who have sex with men who might be at higher risk of infection.
Meningitis vaccine 4CMenB provides 40% protection against gonorrhea
An observational study led by Dr. Winston Abara, of U.S. Centers for Disease Control and Prevention, used health records to identify laboratory-confirmed cases of gonorrhea and chlamydia—another leading STI—among 16–23-year-olds in New York City, NY and Philadelphia, PA, from 2016–2018. These cases were compared with immunization records to determine people’s vaccination status with 4CMenB—which is licensed for use against meningitis—at the time of infection.
There were more than 167,000 infections (18,099 gonorrhea, 124,876 chlamydia, and 24,731 co-infections) among almost 110,000 people. A total of 7,692 people had received the 4CMenB vaccine, with 4,032 (52%) receiving one dose, 3,596 (47%) two doses, and 64 (less than 1%) more than two doses. Full 4CMenB vaccination—receiving two doses—was estimated to provide 40% protection against gonorrhea. One vaccine dose provided 26% protection.
Dr. Winston Abara said: “Our findings suggest that meningitis vaccines that are even only moderately effective at protecting against gonorrhea could have a major impact on prevention and control of the disease. Clinical trials focused on the use of 4CMenB against gonorrhea are needed to better understand its protective effects and could also offer important insights towards the development of a vaccine specifically for gonorrhea.”
The authors acknowledge some limitations. The findings may not be generalisable to wider groups because the data used were from people aged 16–23 years in two large urban settings in the U.S.. Additionally, use of surveillance data means it is possible some participants’ infection and vaccination status were misclassified, affecting the analysis.
Two-dose course of 4CMenB is 33% effective against gonorrhea in adolescents and young adults
South Australia’s ongoing 4CMenB vaccination program is the most extensive globally, initially involving infants, children, adolescents, and young adults with a continuing state-funded program for infants and adolescents. In an observational study led by Professor Helen Marshall, of the Women’s and Children’s Hospital in Adelaide, researchers assessed the effectiveness of 4CMenB against meningitis and gonorrhea as part of an infant, child and adolescent vaccination program.
The authors analyzed meningitis and gonorrhea infection data held by the Communicable Disease Control Branch, and 4CMenB vaccination records from the Australian Immunization Register. To estimate the effectiveness of 4CMenB against gonorrhea, patients diagnosed with chlamydia acted as controls because of similar sexual behavioral risks reported in patients with either infection.More than 53,000 adolescents and young adults received at least one dose of 4CMenB during the vaccination program’s first two years. As well as being highly effective against meningococcal B meningitis and sepsis, in adolescents and young adults a two-dose course of 4CMenB was 33% effective against gonorrhea
Professor Helen Marshall said: “While recent studies have provided evidence that 4CMenB vaccination is associated with reduced risk of gonorrhea, the vaccine was only offered to adolescents and young adults for short periods. The unprecedented scale of South Australia’s 4CMenB vaccination program offers valuable real-world evidence of the vaccine’s effectiveness against meningococcal B meningitis in children and adolescents, and gonorrhea in adolescents and young people. This information is vital to inform global meningitis vaccination programs and policy decisions.”
The authors acknowledge some limitations. While a meaningful reduction in the rate of gonorrhea among adolescents and young adults was not observed, this was likely due to small case numbers in this age group. The reported effectiveness of 4CMenB against gonorrhea is consistent with other studies. Co-infections of gonorrhea and chlamydia may play an important role in disease spread and severity, but factors associated with rates of co-infections are not well understood. However, the analysis shows 4CMenB effectiveness was similar whether co-infections were included or not.
Writing in a linked Comment on both observational studies, Professor Jason Ong, Dr. Magnus Unemo, Annabelle Choong, Victor Zhao, and Dr. Eric Chow, who were not involved in the studies, highlight key measures to adopt while efforts to develop a gonorrhea vaccine continue: “In the meantime, we must continue to strengthen prevention efforts, improve access to early diagnosis and evidence-based treatment (index cases and sexual contacts), ensure quality-assured global surveillance systems to inform treatment guidelines, and invest in rapid, reliable point-of-care tests (for detection of N gonorrhoeae and its antimicrobial resistance) and the development of novel therapeutic antimicrobials.”
Vaccination based on infection risk could prevent 110,000 cases in England and save £8 million over 10 years
Until now, no study has assessed both the health impact and cost-effectiveness of using a vaccine to avert gonorrhea infections.
A modeling study led by Professor Peter White, Imperial College London, UK, is the first analysis of the health and economic effects of using a vaccine to protect against gonorrhea that accounts for its impact on future rates of infection.
A simulation model was developed to compare three realistic vaccination approaches among men-who-have-sex-with-men (MSM) in England: vaccination of all men attending sexual health clinics; vaccination following a confirmed gonorrhea diagnosis; or vaccination based on risk of infection.
Based on their analysis and a balance of cases prevented vs the cost of vaccination, the authors recommend vaccinating MSM at highest risk of gonorrhea infection with 4CMenB, which would prevent an estimated 110,000 cases and save £8 million over 10 years.
Professor Peter White said: “With a gonorrhea-specific vaccine likely to take years to develop, a key question for policymakers is whether the meningitis vaccine 4CMenB should be used against gonorrhea infection. Our analysis suggests that giving the vaccine to those at the greatest risk of infection is the most cost-effective way to avert large numbers of cases.”
The authors explain that their estimation of the benefit of using 4CMenB to protect against gonorrhea is conservative. Due to a lack of data at the time of the study, it was assumed a first vaccine dose offers no protection so only those who received a second dose were protected; however, the study by Abara and colleagues suggests one dose offers some protection, increasing the benefit of vaccination. Additionally, vaccination will reduce the future impacts of antimicrobial resistance (AMR)—which are likely to be substantial—meaning that vaccination would be even more beneficial than currently estimated, but further studies are needed to assess the potential future burden of AMR.
Source: Read Full Article
