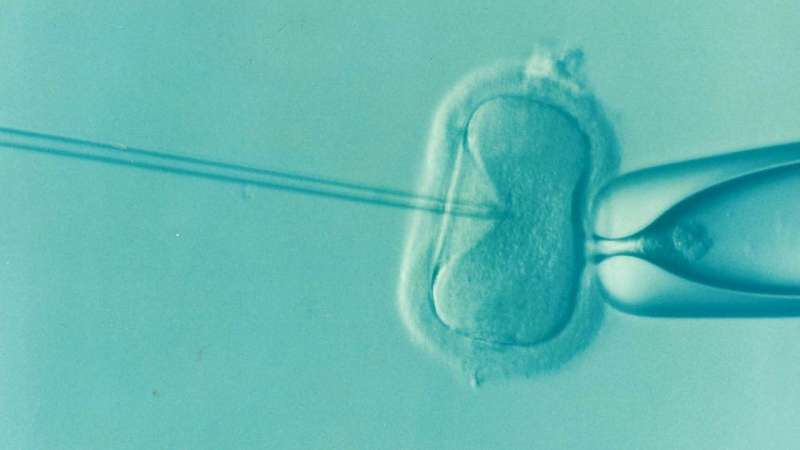
The world’s first IVF baby, Louise Brown born in England in 1978, was conceived from a naturally developing follicle in her mother’s ovary. However, as other groups around the world would quickly discover, the “natural cycle” was an inefficient and difficult procedure to replicate, and most turned to the ‘stimulated’ cycle to provide more eggs for fertilization and a greater chance of pregnancy. Since then, many combinations of fertility hormones have been tried to improve outcomes, but the stimulated cycle remains the cornerstone of today’s IVF.
Now, a new “study of studies,” whose results are presented today at the 38th annual meeting of ESHRE in Milan, has found little or no difference in live birth rate from these various stimulation protocols, but concluded that one group of protocols in particular is likely to reduce the risk of the most serious treatment complication of IVF, ovarian hyperstimulation syndrome, or OHSS. The results of this meta-analysis are presented today on behalf of the Cochrane group by Dr. Pedro Melo from the Tommy’s National Center for Miscarriage Research at the University of Birmingham, UK.
The study was a huge review of randomized trials examining the efficacy and safety of 56 different protocols used in assisted reproduction (IVF and ICSI) and involving almost 37,000 women who were subjects in 171 eligible trials. The headline results showed there is probably “little to no effect” of any of the regimens on live birth rate but that a “short GnRH antagonist protocol” reduced the chance of OHSS by as much as 52% in high-risk subjects when compared with “long GnRH agonist” protocols.
Fertility hormones used for ovarian stimulation—known as gonadotrophins—were originally derived from natural sources and aimed to replicate the activity of natural hormones; human menopausal gonadotrophin, for example, was extracted from the urine of menopausal women. Other preparations have in time become available through genetic manufacturing, such that today “recombinant FSH” (follicle stimulating hormone) is the most commonly used gonadotrophin for ovarian stimulation.
In addition to gonadotrophins, most stimulation cycles also involve the administration of drugs which temporarily shut down the natural ovulatory cycle by suppressing that part of the brain which controls the ovaries (the pituitary gland). Pituitary suppression (or downregulation) drugs are used to prevent early release of the eggs and allow clinicians to better schedule the egg retrieval procedure.
Many different combinations—or protocols—of gonadotrophins and pituitary downregulation drugs are today used for ovarian stimulation in IVF. Downregulation can be achieved with a hormone known as a GnRH agonist (gonadotrophin-releasing hormone). However, downregulation with a GnRH agonist requires several weeks to achieve, and is thus known as a “long protocol.” More recently it was found that a GnRH antagonist suppressed the ovary’s activity much more quickly and reduced the time of the stimulation cycle from five or six weeks to just two or three.
It was this study’s comparison of the long GnRH agonist and the short antagonist protocols which offered its important safety finding. OHSS is a complication most usually found in patients whose ovarian reserve tests suggest a normal or high response to ovarian stimulation. The condition presents with enlargement of the ovaries with abdominal bloating and pain, and may rarely progress to more serious circulatory, respiratory and renal complications. Mild OHSS is common in IVF patients, affecting as many as 33%, but rare (1%) in its serious forms. The evidence from this latest meta-analysis showed that in women with predicted normal or high response the use of short GnRH antagonist protocols resulted in little to no difference in live birth rate but a reduction in OHSS of as much as 52% when compared with long GnRH agonist protocols.
The mechanisms through which short GnRH antagonist protocols reduce the risk of OHSS have not been fully explained, said Dr. Melo. “However,” he added, “it seems likely that this results from a combination of factors—including the absence of an ovarian “flare” effect with GnRH antagonists, and the option of triggering ovulation in GnRH antagonist cycles without hCG (human chorionic gonadotrophin), which is the main driver of OHSS.”
Thus, said Dr. Melo, “we can now say with a good level of confidence that in patients with predicted high or normal response, using long protocols is unlikely to improve their live birth rates but will probably increase their risk of OHSS.”
Source: Read Full Article
